2022-04-14
More and more antibiotics are failing and resistance is spreading around the world. The situation is worst in low-income countries, a new report shows. The situation is acute - but not hopeless.

Escherichia coli. Klebsiella pneumoniae. Staphylococcus aureus. Streptococcus pneumoniae.
Or we could put it this way: bacteria that cause everything from urinary tract infections to life-threatening wound infections. Staphylococci that can lead to life-threatening sepsis. And pneumococcus, which is the most common cause of pneumonia.
These are some of our most common bacteria – and also a few of those that can be linked to most of worldwide deaths from antibiotic resistance.

Waddah 15, during a regular vital signs checkup. He was admitted to the isolation department at MSF Aden hospital after discovering a bacterial infection in his wounds.
MSF established the isolation department at MSF Aden hospital after discovering a high number of bacterial infections between the admitted patients. Photo: Ehab Zawati, MSF. Photo: Ehab Zawati, MSF.
In a new study, published in the medical journal The Lancet, a group of researchers have calculated how many people died as a result of antibiotic-resistant infections in 2019. More than 1.2 million deaths. The situation is worst in low-income countries.
Acute situation

The result? Shocking. But hardly surprising, says Jacob Goldberg, Medical Humanitarian Advisor on antibiotic resistance issues for Médecins Sans Frontières (MSF).
– For a long time we have known that the problem is enormous, even in the places where we work. Previous reports have estimated how many people will die as a result of the development of resistance by 2050. That seemed pretty remote. With this new study, we have a clear picture of how many people are dying now already. I hope this makes the issue more urgent.
Jacob Goldberg, Médecins Sans Frontières
Yes, the situation is urgent. Because what usually remedies the development of drug resistance – that is, the development of new drugs to replace the old ones – does not work when it comes to antibiotics. Instead, now we are a situation where resistance to available antibiotics is constantly worsening while hardly any new antibiotics are coming onto the market.
It is an emergency – yet the figures in the research report are probably just the tip of the iceberg, says Otto Cars, Professor and Senior Advisor, ReAct.

Photo: Paul Odongo, MSF.
– Yes, I think we can assume that the situation is actually even worse. Antibiotic resistance is a silent pandemic. It is a non-disease and as such it does not fit into the global statistics that have a disease focus. But antibiotic resistance threatens to undermine modern health care, cancer treatments, care of premature babies, surgery and much else. Bacteria are everywhere and if we can’t treat them with antibiotics anymore, we’re in trouble.
Antibiotics prescribed unnecessarily
Let us take a detour, to the Central African Republic. A country with barely 300 trained doctors and even fewer nurses. Antibiotics can be bought anywhere – if you do not have a prescription, you can still buy. A well-equipped laboratory, where bacterial cultures can be examined and possible resistance detected, is only available in the capital Bangui. So, people self-medicate, hoping the fever or pain will subside. And any leftover tablets are saved for the next time a family member get sick.
We could also go to India, where healthcare is deregulated and competition is fierce. Any doctor who does not prescribe what the patient wants, which often is antibiotics, risks losing both the patient and his or her good reputation.
This is the situation in many parts of the world. Even in rich countries, around 50% of all antibiotic prescriptions are actually unnecessary, according to Otto Cars. Added to this is the completely irresponsible use of antibiotics in the animal industry in many places.
And slowly but inexorably, this miracle drug is no longer working. In the places where Médecins Sans Frontières works, this is particularly noticeable among people with weakened immune systems, such as people living with HIV. Resistant bacteria also often spread in the context of war injuries. But it is worst among the youngest, explains Jacob Goldberg.
– When we have an outbreak of multi-drug resistant infections in a neonatal ward, it is serious. They are already so weak.
Shortage of new antibiotics
To stop the outbreak, the source must be identified – which requires access to labs and trained staff.
– We often work in conflict zones, in refugee camps and other places where none of these things are available. So, many times we do not even know there’s an outbreak. We only notice that our patients are dying, says Jacob Goldberg and continues:
– Without labs and diagnostic tools, it is difficult to determine what a febrile child is suffering from, whether it is bacteria at all, and if so, which ones.
– The only thing we can do then is so-called empirical treatment, that is, give the child antibiotics without knowing what caused the infection. We still have to do everything we can to save the child’s life.
– Even more people in the world are dying because of a lack of access to antibiotics, than of antibiotic resistance.

This lack of diagnostic tools is a major reason why the development of resistance has been able to skyrocket in low-income countries. Another reason is the lack of new antibiotics. A shortage that, according to Otto Cars, is largely due to the inaction of the outside world.
– The approach to antibiotic drug development has been far too naive.
Otto Cars
The boom of the ’50s, ’60s and ’70s, when we were inundated with new antibiotics and could treat more and more infections, made us think that the problem was solved and research turned its attention elsewhere.
– I do not think the solution is just about developing new antibiotics, says Otto Cars. As long as antibiotics are used, resistance will emerge, it is inevitable because bacteria adapt to their environment. That is why we have to try to slow down the development of resistance and at the same time have a pipeline that pushes out new drugs.
New partnerships needed
In other words – supply must increase and use must decrease in large parts of the world. This is not an easy equation to solve. The scientific difficulties in developing new antibiotics have reduced interest among the big pharmaceutical companies and led most of them to abandon antibiotic research. Another reason is profitability – why invest in drugs that are not intended to be used, or only as a last resort when the older drugs no longer work?
– To speed up development, the public sector must take leadership and build new partnerships between academic researchers, healthcare and industry, says Otto Cars.
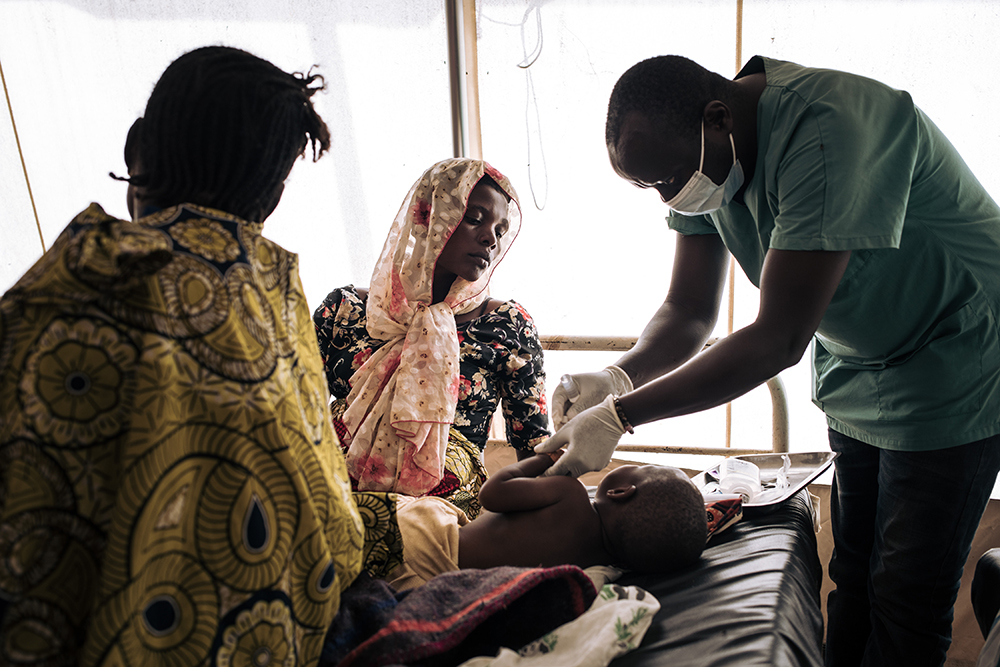
She was admitted the day before because she suffers from diarrhoea, vomiting, cough and high fever. Without a lab, it can be difficult to determine if she needs antibiotics.
Her mother Odette Ngabusi, 23, is a mother of 3. She arrived in Rho one month ago after the attack on her village. Photo: Alexis Huguet, MSF.
The situation is urgent – but not hopeless. For several years, Médecins Sans Frontières has been working systematically to reduce and improve antibiotic use. This includes hand washing and access to clean water, measures that reduce the number of infections and thus the need for antibiotics. Education on responsible use of antibiotics is another part of the work, as is monitoring bacteria and resistance, which in practice means increasing access to labs and diagnostic tools.
Slips under everyone’s radar
Antibiotic resistance is indeed a silent pandemic. It hard to talk loudly about something that is barely visible. Something that for a long time slipped under the radar in the statistics on causes of death and was hidden under headings like “cancer” or “sepsis”.

– Even in low-income countries, governments have found it difficult to see antibiotic resistance as something they want to prioritize and allocate resources to,” says Otto Cars. They have had enough with other diseases, like HIV, tuberculosis and malaria. It becomes a Catch-22 situation – nobody asks for help for a problem they barely know about.
Perhaps the fight against antibiotic resistance will get an unexpected boost – from the COVID pandemic. At least in terms of understanding the importance of access to medicines and diagnostics, Otto Cars continues.
– Of course, we’re all very tired of the pandemic by now, and to start thinking about the next one is not what we want. But we have seen how quickly diagnostic tools and even vaccines can be made available. We have also seen the weaknesses of health systems, the lack of solidarity. As with COVID, we need to recognize that antibiotic resistance is a global problem and if we are to have a chance, we need to take global responsibility now.
Article written by: Åsa Nyquist Brandt, Médecins Sans Frontières.
The article was first published in MSF Sweden’s magazine and then on their website.
Read article on MSF Sweden’s website (in Swedish).
More from "2022"
- 15 things that need to happen in 2023 – for a robust response on antibiotic resistance!
- 7.7 million people die from bacterial infections every year
- ReAct highlights during World Antimicrobial Awareness Week 2022
- Awareness walk in Lusaka, Zambia
- ReAct Asia Pacific: Competitions, webinars, social media campaigns and new Indonesian declaration on AMR
- Otto Cars awarded Research!Sweden’s Honorary Award
- Innovate4Health: 16 finalists from 12 countries!
- Otto Cars has dedicated his life to the fight against antibiotic resistance
- ReAct activities for World Antimicrobial Awareness Week 2022
- ReAct Asia Pacific: Antibiotic Smart Communities as a way forward
- Webinar ReAct Asia Pacific! Moving towards an Antibiotic Smart Community – the use of a novel indicator framework
- Join ReAct Latin America Meeting: Empowered Communities!
- The impact of antibiotic resistance on cancer treatment, especially in low-and middle-income countries, and the way forward
- Sweden: Pernilla’s 8-day old daughter died from sepsis – caused by resistant bacteria Klebsiella
- Five challenges that governments need to address in resolving the stagnation in antibiotic development
- The monkeypox outbreak: Need for antibiotic stewardship?
- Key takeaways from the ReAct Africa and South Centre Conference
- New ReAct Europe and EPHA position paper on EU incentives for new antibiotics development
- Launch of a new approach to antimicrobial stewardship in Zambia
- Time to register for the annual ReAct Africa and South Centre conference!
- Innovate4Health 2022: Call for student team applications!
- “Need to address the paradox of hospitals spreading disease” says new WHO report
- 5 takeaways from AMR Stockholm+50 event
- Student Tehseen Contractor
- ReAct Latin America: call to governments on the use of antimicrobials in intensive animal husbandry
- Join ReAct Stockholm+50 associated event! Global AMR response – What needs to be done?
- New opportunities for global action on AMR?
- Public hearings on elements to be included in a new international instrument on pandemic preparedness & response
- Policy briefing on WHO GAP AMR: 8 pillars of action to address global solutions to AMR
- India: State Action Plans on AMR in focus at stakeholder colloquium
- The silence is killing us – time to listen to the facts
- Access to clean water – a fairly inexpensive way to avoid infections
- Anna Sjöblom new Director ReAct Europe
- Dr. Hari Paraton: Drug resistance bacteria threatens lives of mothers and newborns
- Antibiotic resistance claims more than 1,2 million lives a year, says new large study
- Artificial intelligence – the future of antibiotic resistance prevention?
