2019-10-17
This year’s theme for the International Day for the Eradication of Poverty, on 17 October, is “Acting together to empower children, their families and communities to end poverty”. 2019 also marks the 30th anniversary of the adoption of the Convention on the Rights of the Child (UNCRC), which recognizes every child’s rights to a standard of living adequate for child’s physical, mental, spiritual, moral and social development.
Antibiotic resistance worsens an already high burden of infectious diseases among the poor. Antibiotic resistance and lack of access to effective antibiotics threaten children’s development or can unravel the important achievements in children’s rights.

Disproportionate effect of antibiotic resistance on children and their families in poverty
Antibiotic resistance worsens an already high burden of infectious diseases among the poor. Even though great progress has been made in child health over the past two decades, roughly 3 million newborns and 1.2 million children under five suffer from sepsis every year, which causes over half a million deaths. Children in low- and middle-
income countries face even greater risk where 35%-40% of newborn deaths in south Asia and sub-Saharan Africa were caused by severe bacterial infections.
Antibiotic resistance and lack of access to effective antibiotics threaten children’s development or can unravel the important achievements in children’s rights, thereby jeopardizing the global efforts in empowering children and ending poverty. It is estimated that 214,000 newborn babies die due to bacteria that are resistant to available antibiotics. At the same time, at least 445,000 children in low- and middle-income countries die due to the lack of universal access to effective antibiotics.
More difficult to prevent antibiotic-resistant infections for children in poor families
Children in poor families are also less able to prevent antibiotic-resistant infections. Families living in poverty often lack access to safe drinking water, sanitation and hygiene, and healthcare services. This, in combination with poor nutrition and suboptimal housing conditions, puts poor families and communities at greater risk of contracting infectious diseases.
In the cases where people do have access to healthcare, up to 90% of the population in low-income countries are paying for their healthcare out-of-pocket. This translates to around 25%-70% of total income being spent on healthcare, making medicines the largest family cost after food. Antibiotic resistance adds to these costs in several ways where treatment of resistant infections may:
- depend upon second and third line antibiotics that are often far more expensive,
- take longer to treat and have less chances of success, and
- require hospitalization that, with alternative antibiotics, would not have been necessary.
All of these put an additional strain on household incomes.
The paired burden of poverty and infectious diseases affects more than children’s survival and health. Poor families may attempt to self-medicate their children or see traditional or unqualified practitioners, rather than seeking the help of qualified healthcare professionals. This increases the risk of inappropriate use of antibiotics, which drives resistance in their families and communities. Resistance will further elevate the families’ financial hardship that leads to severe consequences for children’s growth, education and potential for development. Children growing up in poverty suffer more barriers to thrive in school due to illness, financial stress to afford education, transportation, or school absences due to family labor burdens.
Addressing antibiotic resistance and poverty alleviation should go hand-in-hand to ensure the wellbeing of the next generation. Children should have the right to, not only survive, but grow, develop and thrive with sufficient resilience against various global challenges including poverty, antibiotic resistance, climate change, etc.
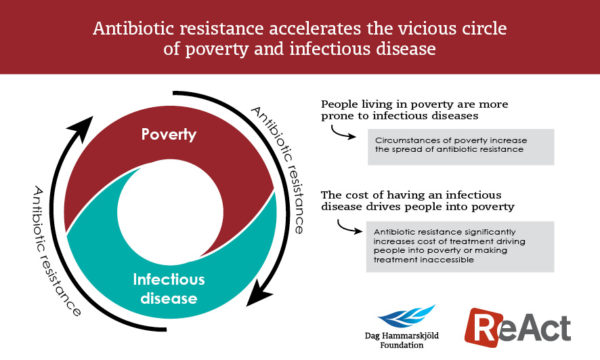
Antibiotic resistance links to poverty
According to the World Health Organization, infectious diseases were responsible for the death of more than 8.4 million people worldwide in 2016. Economically disadvantaged people living in low- and middle-income countries suffered the majority of these deaths.
The World Bank report projects that 24.1 million people could fall into extreme poverty by 2050 because of antimicrobial resistance (including resistance in malaria and HIV). A vast majority of these would live in low- and middle-income countries. The devastating impact of antibiotic resistance at the individual household level and to communities would endanger efforts made to reach SDG 1 – to end poverty in all its forms by 2030.
There is no doubt that access to working antibiotics has played an important role in the overall reduced rates of mortality and morbidity from infectious diseases in low- and middle-income countries over the last decades. Affordable and working antibiotics are essential to those most marginalized and impoverished to live healthier and more productive lives. Poverty alleviation strategies that are sensitive to antibiotic resistance could reduce the vicious circle of infectious disease and poverty.
References
International Day for the Eradication of Poverty 2019
When the Drugs Don’t Work: Antibiotic Resistance as a Global Development Problem
R. Laxminarayan & R. R. Chaudhury, ‘Antibiotic Resistance in India: Drivers and Opportunities for Action’, PLOS Medicine 13, (2016): e1001974.
C. Fleischmann-Struzek et al, “The global burden of paediatric and neonatal sepsis: a systematic review”, The Lancet Respiratory Medicine 6, (2018): 223–230.
R. Laxminarayan et al, “Access to e ective antimicrobials: a worldwide challenge”, Lancet 387, (2016): 168–175.
D. Dharmapalan, A. Shet,V.Yewale & M. Sharland, “High Reported Rates of Antimicrobial Resistance in Indian Neonatal and Pediatric Blood Stream Infections”,
J Pediatric Infect Dis Soc 6, (2017): e62–e68.
I. Ahmed et al, “Population-based rates, timing, and causes of maternal deaths, stillbirths, and neonatal deaths in south Asia and sub-Saharan Africa: a multi-country prospective cohort study”, The Lancet Global Health 6, (2018): e1297–e1308.
A. Cameron, M. Ewen, D. Ross-Degnan, D. Ball & R. Laing, “Medicine prices, availability, and affordability in 36 developing and middle-income countries: a secondary analysis'” Lancet 373, (2009): 240–249.
WHO/HAI Database of medicine prices, availability, affordability and price components
More news and opinion from 2019
- ReAct’s 2019 wrap up and 2020 expectations
- Blog post by UNDP and ReAct: Antimicrobial resistance: An emerging crisis
- Water, sanitation and hygiene services critical to curbing antibiotic quick fix
- Diagnostics: Antibiotic susceptibility
- ReAct highlights during World Antibiotic Awareness week 2019
- 2019 AMR photo competition prizes announced
- Launch of UNICEF’s institutional guidance on antimicrobial resistance
- Proposed ban on colistin for animal use announced in Indonesia
- School children led celebration of World Toilet Day and World Antibiotic Awareness Week
- 10 Innovate4AMR-winning teams enjoyed 3-day workshop in Geneva
- After 4 collaborative meeting days: Actions for the future in Latin America
- Four key points from joint comments to One Health Global Leaders Group on AMR
- Why are children more vulnerable to AMR?
- Dr Yoel Lubell, Health Economist, on Thailand, AMR, UCH and cultural factors driving AMR
- UHC and AMR: The Thai Experience
- Why do effective antibiotics matter for quality of care and patient safety?
- New ReAct policy brief: Antimicrobial resistance and universal health coverage – What’s the deal?
- Three key takeaways from the ReAct Africa conference
- Diagnostics: Species identification
- AMR-specific indicator proposed for monitoring Sustainable Development Goals
- Five focus areas at the 2nd Ministerial Conference on AMR hosted by the Netherlands
- Safety concerns of fecal microbiota transplants
- Upcoming ReAct Africa Conference: universal health coverage and antimicrobial resistance in focus
- Mother Earth conference in Argentina – the environment in focus
- Diagnostics: What are we talking about?
- Connecting global to local civil-society-agenda on AMR at CSO convening in Geneva
- ReAct colleagues featured in WHO Bulletin as leading profiles in the work on reacting to antibiotic resistance
- RAN stakeholder at WHO IPC consultation – for standards and guidelines in African Union member states
- WHA conversation on Antibiotic Resistance as a Global Development Problem co-organized by ReAct
- Insights from ReAct Asia Pacific project on antibiotic stewardship in secondary level hospitals in India
- Open letter to UN Member States from former IACG members Anthony So and Otto Cars
- ReAct UHC Intervention at UNGA Multi-stakeholder Hearing for High-level Meeting on UHC
- ReAct Latin America honors Earth Day
- Medicines Patent Pool’s view on the role of licenses for antibiotics – World Intellectual Property Day
- Second time for Innovate4AMR competition!
- World Health Day 2019: Universal Health Coverage
- Diagnostics: Constraints for successful implementation
- Antibiotic Shortages: magnitude, causes and possible solutions: A new WHO meeting report
- Erry Setyawan, FAO, on Indonesian NAP: We need to work together to make it possible to manage AMR
- ReAct’s new 5-year strategic plan receives funding from Sida
- How infections spread and how to stop them
- Generating data for policy and practice