2026-03-26
As World Health Day approaches on 7th April, there's no better time to reflect on one of medicine's most pivotal achievements: the discovery and mass production of penicillin. While this miracle drug has been a beacon of hope for 80 years, saving countless lives, its future is under siege. Understanding the precarious position of this breakthrough is not just an exercise in medical history; it's a call to action for the preservation of modern healthcare itself.

Life before antibiotics
The discovery of penicillin by Sir Alexander Fleming in 1928 remains one of the most critical turning points in human history. To truly appreciate penicillin, we must first look back at the pre-antibiotic era. At the start of the 20th century, infections were the leading cause of death. In the U.S. in 1900, infectious diseases caused one-third of all mortality, with pneumonia, tuberculosis, and diarrheal diseases as the top killers .
Simple events like a minor cut, an insect bite, or childbirth frequently led to fatal infections. In many major conflicts,, more soldiers succumbed to infected wounds than to combat itself. While pioneers like Pasteur and Lister had established the germ theory and improved hygiene, it was the introduction of effective antibiotics, starting with penicillin’s mass production in the 1940s, that truly changed the odds.
How penicillin transformed medicine

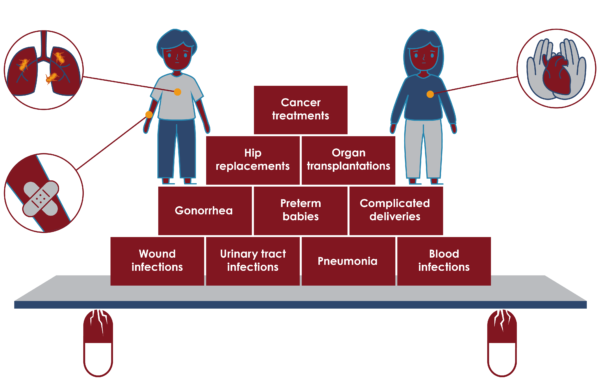
Penicillin and the subsequent development of other antimicrobials didn’t just treat sickness; they enabled entirely new fields of medicine. This transformation can be seen in several key areas:
Wound management
Previously life-threatening injuries became manageable concerns overnight. Infections like sepsis, once a death sentence, could now be successfully treated, transforming battlefield and industrial medicine.
Maternal and child health
Infections remain a major killer of mothers and children in low-income nations, but in high-income countries, antibiotics drastically reduced mortality associated with childbirth and common childhood illnesses, such as pneumonia, diarrhoea, and severe ear or throat infections.
Sexually transmitted Infections
Antibiotics also transformed the treatment of common STIs such as syphilis and gonorrhoea, which previously caused severe long-term health consequences and widespread transmission.
Complex surgeries
Modern surgery, including procedures like hip replacements and organ transplants, is completely dependent on antibiotics to prevent lethal post-operative infections. Without them, the risk of infection would outweigh the benefit of most complex operations.
Critical care and immunosuppression
Intensive care units (ICUs) and treatments for cancer (chemotherapy) or autoimmune diseases rely on the ability to prevent or quickly treat infections in highly vulnerable, immunosuppressed patients
The looming threat and the path forward
Despite its remarkable success, this medical revolution is fragile. The vision of a post-antibiotic world is bleak: a massive decrease in global life expectancy, ordinary infections becoming untreatable and fatal, and major procedures like chemotherapy and organ transplantation being rendered impossible. Current estimates suggest that antibiotic resistance causes over 1.2 million deaths each year , and projections indicate this could rise dramatically by 2050 without urgent action .
Preserving the legacy of penicillin requires a complex, multi-faceted, whole-of-society strategy that addresses global equity. On one hand, we must focus on the sustainable use of existing drugs, reducing unnecessary consumption in both human and animal health to slow the development of resistance. On the other, we must urgently tackle the issue of access, ensuring that the millions in poorer countries who still lack these life-saving medicines receive them.
Furthermore, we must support the development of new antibiotics, diagnostics, vaccines, and alternative therapies, alongside stronger prevention measures — from infection control and vaccination to Water, Sanitation and Hygiene (WASH) – and a more efficient end-to-end pipeline to bring these tools to those who need them. Only through coordinated global action can we ensure that future generations continue to benefit from one of medicine’s greatest breakthroughs.
More from "2026"
- The Abuja turning point: Renewing ambition and accountability needed to deliver practical outcomes for the global AMR response
- ReAct Europe at the 2026 Nobel Prize Teacher Summit: Global health in focus
- Securing the future of health: ReAct Latin America and Idec propose a new regional strategy for the Americas
- World Health Day: Reflecting on the penicillin revolution
- Reimagining AMR action through community voices: Lessons from Jahangirpuri, New Delhi, India
- Are you our new Director for ReAct Latin America?
- ¿Eres nuestra nueva Directora o Director de ReAct Latinoamérica?
- Share your perspective: Community priorities survey for the Abuja 2026 AMR Ministerial Meeting
- School gardens to contain AMR: Belén Juca’s experience with children in Ecuador
- ReAct at first Regional Meeting on AMR in Brasilia
- Faith Based Organizations: Critical allies for stronger action on AMR
- From Declaration to Action: Insights from the ReAct Asia Pacific 2025 Conference Report
- Antibiotic resistance and aquaculture: Why It matters for One Health
- Revised Global Action Plan on AMR delayed over technology transfer language
- Reflections from the EU JAMRAI2 Annual Meeting
- ReAct Latin America at global AMR Summit in Costa Rica
- A regional anthology: 20 years of action on antibiotic resistance
- Mobilizing faith-based organizations to address antibiotic resistance in Africa
- India’s AMR Response: High-level leadership and Implementation challenges
- Protecting cancer care in the age of antibiotic resistance
- BRIDGE-ABR: A ReAct-led collaboration on goal conflicts, antibiotic resistance and sustainability